Cellulitis
Description of Medical Condition
This is an acute, spreading infection of the dermis and subcutaneous tissue. Several entities are recognized:
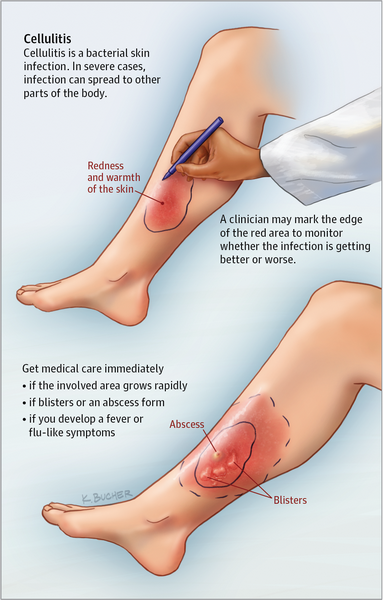
- Cellulitis of the extremities - characterized by an expanding, red, swollen, tender, or painful plaque with an indistinct border that may cover a wide area
- Recurrent cellulitis of the leg after saphenous venectomy - patients have an acute onset of swelling and erythema of the legs that develops months to years after coronary artery bypass. (This surgery uses lower-extremity veins for bypass grafts.)
- Dissecting cellulitis of the scalp - recurrent, painful, fluctuant dermal and subcutaneous nodules
- Facial cellulitis in adults - a rare event. Patients usually develop pharyngitis followed by high fever, rapidly progressive anterior neck swelling, tenderness, and erythema associated with dysphagia.
- Facial cellulitis in children - potentially serious. Swelling and erythema of the cheek develop rapidly, usually on one side.
- Perianal cellulitis - bright perianal erythema extending from the anal verge approximately 2.5 cm (1 in) onto the surrounding perianal skin
- Pseudomonas cellulitis - this may be a localized phenomenon, or it may occur during Pseudomonas septicemia
| Type | Typical location | Key clinical features |
|---|---|---|
| Cellulitis of the extremities | Arms and legs | Expanding, red, swollen, tender, or painful plaque with poorly defined borders |
| Recurrent cellulitis of the leg after saphenous venectomy | Lower extremity at vein harvest site | Acute swelling and erythema months to years after coronary artery bypass surgery |
| Dissecting cellulitis of the scalp | Scalp | Recurrent painful nodules with purulent drainage and interconnecting abscesses |
| Facial cellulitis in adults | Face and anterior neck | Pharyngitis followed by high fever, rapidly progressive neck swelling, tenderness, and erythema |
| Facial cellulitis in children | Cheek, usually one side | Rapidly developing unilateral facial swelling and erythema |
| Perianal cellulitis | Perianal skin | Bright erythema extending outward from the anal verge with pain and pruritus |
| Pseudomonas cellulitis | Variable | Localized skin infection or a manifestation of Pseudomonas septicemia |
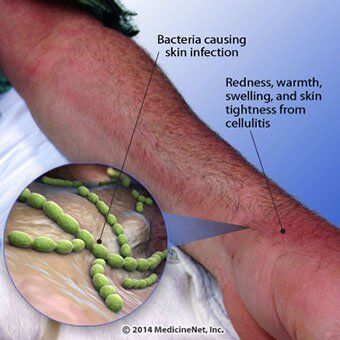
System(s) affected: Skin/Exocrine
Genetics: No known genetic pattern
Incidence/Prevalence in the US: Unknown
Predominant age:
- Perianal cellulitis - mainly in children
- Facial cellulitis - in adults, usually older than 50 years. In children, it occurs between 6 months and 3 years.
Predominant sex: Male = Female (perianal cellulitis is more common in boys)
Medical Symptoms and Signs of Disease
General
- Local tenderness
- Pain
- Erythema
- Malaise
- Fever, chills
- The involved area is red, hot, and swollen
- The borders of the affected area are not elevated and are not well demarcated
- Regional lymphadenopathy is common
Recurrent cellulitis
- Same as above
- Edema
- High fever, chills, and toxicity
Recurrent episodes may reflect underlying risk factors such as prior surgery, lymphedema, or chronic skin breakdown, and warrant careful evaluation for modifiable triggers.
Dissecting cellulitis of the scalp
- Purulent drainage from burrowing, interconnecting abscesses
Facial cellulitis in adults
- Malaise
- Anorexia
- Vomiting
- Itching
- Burning
- Dysphagia
- Anterior neck swelling
Facial cellulitis in children
- Irritability
- Upper respiratory tract infection symptoms
Perianal cellulitis
- Intense perianal erythema
- Pain on defecation
- Blood-streaked stools
- Perianal pruritus
What Causes Disease?
By site
- Cellulitis of the extremities: Group A Streptococcus, Staphylococcus aureus
- Recurrent cellulitis of the leg: Non-group A beta-hemolytic streptococci (group C, G, B)
- Dissecting cellulitis of the scalp: Staphylococcus aureus
- Facial cellulitis in adults: H. influenzae type B
- Facial cellulitis in children: H. influenzae type B; in children over 3 years, with a portal of entry:
- staphylococcal and streptococcal
- Synergistic necrotizing cellulitis: Mixed aerobic-anaerobic flora
- Intravenous drug use: Staphylococcus aureus. Streptococci, Enterobacteriaceae, Pseudomonas, fungi
- Synergistic necrotizing cellulitis: Mixed aerobic-anaerobic flora
Specific diseases
- Diabetes mellitus: Staphylococcus aureus.
Streptococci, Enterobacteriaceae, anaerobes
- Human bites: Eikenella corrodens
- Animal bites (cat and dog): Staphylococci, Pasteurella multocida
Patient groups
Neonates: Group B Streptococcus; immunocompromised
- Bacteria (Serratia, Proteus, and other Enterobacteriaceae)
- Fungi (Cryptococcus neoformans)
- Atypical mycobacterium
- Children with nephrotic syndrome: E. coli
- Environmental and occupational exposures
- Erysipelothrix rhusiopathiae
Vibrio species
- Aeromonas hydrophila
Rare causes
- Anaerobic
- Clostridium perfringens (gas-forming cellulitis)
- Tuberculosis
- Syphilitic gumma
- Fungal: Mucormycosis, Aspergillosis
Risk Factors
General
- Previous trauma (laceration, puncture, human or animal bite)
- Underlying skin lesion (furuncle, ulcer)
- Surgical wound
- Recurrent cellulitis
- After coronary artery bypass in patients whose saphenous veins have been removed
- Lower extremity lymphedema secondary to (a) radical pelvic surgery (b) radiation therapy (c) neoplastic involvement of pelvic lymph nodes
- Mastectomy
- Diabetes mellitus
- Intravenous drug use
- Immunocompromised host
- Burns
- Environmental and occupational factors
| Risk factor category | Examples | Supportive measures |
|---|---|---|
| Skin barrier disruption | Trauma, lacerations, puncture wounds, ulcers, burns, surgical wounds | Prompt cleansing, wound care, and monitoring for redness, warmth, or swelling |
| Edema and impaired lymphatic drainage | Lower extremity lymphedema, post-mastectomy changes | Compression as advised, leg elevation, and skin moisturization to reduce cracking |
| Systemic conditions | Diabetes mellitus, immunocompromised states, nephrotic syndrome | Careful glycemic and disease control and early evaluation of any skin infection |
| Environmental and exposure risks | Occupational exposures, fresh or salt water contact with skin breaks, human or animal bites | Avoid contaminated water with open wounds and seek care promptly after bites |
| Recurrent cellulitis | History of prior episodes | Attention to prevention strategies and discussion of prophylaxis with a healthcare provider |
Diagnosis of Disease
Differential Diagnosis
Perianal cellulitis or Candida intertrigo
- Psoriasis
- Pinworm infection
- Inflammatory bowel disease
- Behavioural problem
- Child abuse
Others
- Acute gout
- Fasciitis/myositis
- Mycotic aneurysm
- Ruptured Baker's cyst
- Thrombophlebitis
- Osteomyelitis or herpetic whitlow
- Cutaneous diphtheria
- Pseudogout
Laboratory
- Aspirates from the point of maximum inflammation yield a 45% positive culture rate, compared with 5% from leading-edge culture.
- Blood cultures - potential pathogens are isolated in 25% of patients
- Mild leukocytosis with a left shift
- A mildly elevated sedimentation rate
- Complete blood count (CBC)
Drugs that may alter lab results: Previous antibiotic therapy may alter the results
Disorders that may alter lab results: N/A
Laboratory findings support the diagnosis and help identify the causative organism, but the clinical picture and progression of skin findings remain central to management.
Pathological Findings
Skin biopsy shows marked infiltration of the dermis with eosinophils and inflammatory changes.
Special Tests
- Serial serological testing with antistreptolysin O, anti-deoxyribonuclease B, and anti-hyaluronidase tests may be successful in diagnosing cellulitis caused by group A, C, or G hemolytic streptococci
- Sinus drainage and culture of aspirate
Imaging
Gas-forming cellulitis
- Plain X-rays show gas bubbles in the soft tissue
- CT shows gas and myonecrosis
Diagnostic Procedures
- Skin biopsy
- Lumbar puncture should be considered for all children with H. influenzae type B cellulitis
Decisions about diagnostic procedures, including lumbar puncture, should be made by the treating clinician based on age, symptoms, and overall risk of invasive disease.
Treatment (Medical Therapy)
Appropriate Health Care
Outpatient care is appropriate for mild cases, and inpatient care is appropriate for severe infections.
The choice between outpatient and inpatient care depends on the extent of infection, systemic symptoms, comorbidities, and the patient's ability to adhere to treatment and follow-up.
General Measures
- Immobilization and elevation of the involved limb to reduce swelling may be needed in H. influenzae type B cellulitis
- Sterile saline dressings to decrease local pain
- Moist heat to localize the infection
- Cool aluminum acetate (Burow's solution) compresses for pain relief
Surgical Measures
- Debridement for gas or purulent collections
- Intubation or tracheotomy may be needed for cellulitis of the head or neck
- Hand infections - a wide filleting incision in necrotizing cellulitis
Activity
Ambulatory in mild infection; bed rest in severe infection
Diet
Regular diet
Patient Education
- Good skin hygiene
- Avoid skin trauma
- Report early skin changes to a physician
Patients should be advised to complete the full course of antibiotics as prescribed, attend follow-up visits, and seek prompt care if redness, pain, fever, or systemic symptoms worsen despite treatment.
Medications (Drugs, Medicines)
Drug(s) of Choice
Treat for 10-30 days. Use culture results to guide therapy whenever possible.
- Mild early suspected streptococcal etiology: aqueous penicillin G, 600,000 U, then IM procaine penicillin at 600,000 U q8-12 hrs
- Staphylococcal infection or no clues to etiology: penicillinase-resistant penicillin (e.g., oxacillin 0.5-1.0 g po q6 hrs)
- Severe infection: penicillinase-resistant penicillin (e.g., nafcillin 1.0-1.5 g IV q4 hrs)
- Gram-negative bacillus as possible etiology: aminoglycoside (gentamicin) plus a semisynthetic penicillin
- Rapidly progressive cellulitis after a fresh-water injury: penicillinase-resistant penicillin plus gentamicin or chloramphenicol
- Human bites: amoxicillin-clavulanate (Augmentin)
- Animal bites (cellulitis at the saphenous site): penicillin or nafcillin, in high dosage, IV for 7 days before switching to oral therapy
- Facial cellulitis in adults and children: (H. influenzae type B) cefotaxime IV
- Gas-forming cellulitis: aqueous penicillin G 10-20 million U/day IV
- Diabetes mellitus: cefoxitin or, if toxic, clindamycin and gentamicin
- Intravenous drug abuse: vancomycin and gentamicin
- Compromised hosts: clindamycin and gentamicin
- Burn patients: vancomycin and gentamicin
Contraindications: Allergy to the antibiotic
Precautions: Renal failure, other organ failure
Significant possible interactions: Refer to the manufacturer's literature
Antibiotic selection and duration should be individualized by a healthcare provider, taking into account local resistance patterns, organ function, concomitant medications, and any history of drug allergy.
Alternative Drugs
Mild infection
- Penicillin allergy: erythromycin, 500 mg po q6 hrs
Severe infection
- Vancomycin 1.0-1.5 g/day IV
- Human bites and animal bites: IV cefoxitin
Gas-forming cellulitis
- Metronidazole 500 mg IV q6h
- Clindamycin 600 mg IV q8h
Fluoroquinolones (adults)
Fluoroquinolones are generally reserved for adults and should be prescribed and monitored by a clinician familiar with their indications, adverse effects, and potential drug interactions.
Patient Monitoring
- A blood culture at the end of treatment to ensure cure
- Repeat needle aspirate culture
- Repeat blood count if the patient was toxic
- Repeat lumbar puncture in case of meningitis
Prevention / Avoidance
- Treatment of tinea pedis with an antifungal (such as clotrimazole) will prevent recurrent cellulitis of the legs in patients who have had coronary bypass
- Avoid trauma
- Avoid swimming in fresh water or salt water if a skin abrasion is present
- Avoid human or animal bites
- Support stocking with peripheral edema
- Good skin hygiene
- For recurrent cellulitis - prophylactic penicillin G (250-500 mg po bid)
- H. influenzae cellulitis - rifampin prophylaxis for the entire family of the index case, or in the day care classroom in which one or two children have been exposed. Dosage: 20 mg/kg/day (maximum: 600 mg/day) for 4 days.
Preventive strategies focus on protecting the skin barrier, promptly treating minor infections such as tinea pedis, and considering prophylactic regimens in carefully selected patients under specialist guidance.
Possible Complications
- Bacteremia
- Local abscesses
- Superinfection with gram-negative organisms
- Lymphangitis, especially in recurrent cellulitis
- Thrombophlebitis of the lower extremities in older patients
- Dissecting cellulitis of the scalp - scarring; alopecia
- Facial cellulitis in children - meningitis in 8% of patients
- Gas-forming cellulitis - gangrene; amputation; 25% mortality
Expected Course / Prognosis
With adequate antibiotic treatment, the outlook is good.
Prompt recognition and treatment help reduce the risk of complications. Patients should seek urgent medical attention if fever, rapidly spreading redness, severe pain, or systemic symptoms develop or worsen.
Miscellaneous
Associated Conditions
Facial cellulitis in children
- Upper respiratory tract infection
- Unilateral or bilateral otitis media in 68% of patients
- Meningitis in 8% of patients
Perianal cellulitis
- Pharyngitis may precede the infection
Frontal sinus in adult or subacute bacterial endocarditis
- Scarlet fever
- Vaccinia
- Herpes simplex
- Herpes zoster
Age-Related Factors
Pediatric: N/A
Geriatric: In cellulitis of the lower extremities, patients are more likely to develop thrombophlebitis
Pregnancy
N/A
International Classification of Diseases
682.9 Cellulitis and abscess at unspecified site

















