Mebendazole

Dosages
Mebendazole 100 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 90 | C$0.69 | C$62.28 | |
| 120 | C$0.63 | C$76.13 | |
| 180 | C$0.58 | C$103.81 | |
| 270 | C$0.54 | C$145.33 | |
| 360 | C$0.52 | C$188.24 |
Payment & Shipping
Your order is carefully packed and ships within 24 hours. Here is what a typical package looks like.
Sized like a regular personal letter (approximately 24x11x0.7 cm), with no indication of what is inside.



| Shipping Method | Estimated delivery |
|---|---|
| Express Free for orders over C$415.23 | Estimated delivery to Canada: 4-7 days |
| Standard Free for orders over C$276.82 | Estimated delivery to Canada: 14-21 days |








Discount Coupons
- Canada Day - July 1, 2026 10% CANADADAY10
- Boxing Day - December 26, 2026 12% BOXING12
Brand Names
| Country | Brand Names |
|---|---|
 Argentina Argentina | Dazomet Helmint Mebutar Nemasole Tesical |
 Australia Australia | Chemists Own De Worm Sqworm |
 Belgium Belgium | Docmebenda |
 Brazil Brazil | Ascariobel Ascaritor Ascarobex Athelmin Averpan Belmirax Bendrax Bivalem Certovermil Cessaverm Crisdazol Divermil Ductelmin Eraverm Feller Geophagol Gran-Verm Helmizil Ibdazol Kindelmin Meben Mebendazotil Mebendil Mebental Mebiozol Medazol Menbel Moben Multielmin Multizol Necamin Neo Mebend Novelmin Panfugan Pantelmin Panverm Paraverm Parelmin Pentazole Pluriverm Plurivermil Polidazol Politelmin Probendazol Quintelmin Sifbem Sirben Tetrahelmin Trotil Vermepen Vermiben Verminon Vermirax Vermonon Vermoplex Vermoral Verzol Zol-Triq Zoldaben |
 Germany Germany | Surfont |
 Greece Greece | Cecurin Septinalis |
 Malaysia Malaysia | Quemox Thelmox |
 Mexico Mexico | Amatol Amycil Benedaxol Bensolmin Bestelar Carbatil Daben Diazolen Edivertin Exaverm Exbenzol Exteny Fanciadazol Hedazol Helminzole L-Ombrix Lumbicid M-Bentabs Marben Meb-Overoid Meban Mebandozer Mebelmin Mebendicin Mebensole Mebentiasis Mebentine Mebentral Mizolmex Nemapres Oxizole Panvermin Paranzol Prodazol Profenzol Revapol Soltric Vermicol Vermidil Vermin-Dazol Vertex Vertizole |
 Netherlands Netherlands | Anti-Worm Kruidvat Anti-worm Madicure Trekpleister Anti-Worm |
 New Zealand New Zealand | Combantrin-1 Mindol |
 Portugal Portugal | Pantelmin Toloxim |
 Spain Spain | Bantenol Lomper Mebendan Oxitover Sufil Sulfil |
 Turkey Turkey | Vermazol Versid |
| Manufacturer | Brand Names |
|---|---|
| Cipla Limited | Mebex |
Description
Mebendazole is a synthetic anthelmintic medicine that is structurally related to albendazole and thiabendazole.
Uses
Because it works against a broad range of worms, mebendazole can be useful for treating mixed helminth infections. It has produced egg reduction rates and/or cure rates of over 90% in patients with enterobiasis, ascariasis, or hookworm infection caused by A. duodenale or N. americanus, and egg reduction rates of over 90% with cure rates of about 70% in patients with trichuriasis.
How well mebendazole works for helminth infections can vary depending on factors such as pre-existing diarrhea, GI transit time, the degree of infection, and the helminth strain. Cure rates are usually lower than average in patients with very heavy infections and in those with increased GI motility.
Although other anthelmintics, such as praziquantel and albendazole, are usually recommended for infections caused by cestodes (tapeworms), mebendazole has also been used to treat intestinal infections caused by the adult forms of certain tapeworms, including Hymenolepis nana (dwarf tapeworm), Taenia saginata (beef tapeworm), and T. solium (pork tapeworm), as well as hydatid disease caused by the larval form of Echinococcus granulosus (dog tapeworm).
Nematode (Roundworm) Infections
Ascariasis
Mebendazole is used to treat ascariasis caused by Ascaris lumbricoides. Albendazole, mebendazole, or pyrantel pamoate are considered the drugs of choice for ascariasis.
Enterobiasis
Mebendazole is used to treat enterobiasis caused by Enterobius vermicularis (pinworm). Albendazole, mebendazole, or pyrantel pamoate are considered the drugs of choice for enterobiasis.
Filariasis
Mebendazole or albendazole are considered the drugs of choice for filariasis caused by Mansonella perstans. Mebendazole has also been used to treat onchocerciasis (filariasis caused by Onchocerca volvulus), but ivermectin is usually considered the drug of choice for this infection. Other anthelmintics, usually diethylcarbamazine, are recommended for infections caused by most other filarial worms; in Canada, access may be through specialized public health or special access channels.
Hookworm Infections
Mebendazole is used to treat intestinal hookworm infections caused by Ancylostoma duodenale or Necator americanus, whether the infection occurs alone or together with other worms. Albendazole, mebendazole, or pyrantel pamoate are considered the drugs of choice for intestinal hookworm infections. Mebendazole has also been used to treat cutaneous larva migrans (creeping eruption) caused by dog and cat hookworms. However, cutaneous larva migrans usually clears on its own after several weeks or months, and other drugs, such as albendazole, ivermectin, or thiabendazole, are usually recommended if treatment is needed. Mebendazole, albendazole, or pyrantel pamoate are considered drugs of choice for eosinophilic enterocolitis caused by Ancylostoma caninum (dog hookworm).
Toxocariasis (Visceral Larva Migrans)
Mebendazole is used to treat toxocariasis (visceral larva migrans) caused by Toxocara canis or T. cati (dog and cat roundworms), and albendazole or mebendazole are considered the drugs of choice for these infections. In severe cases with cardiac, ocular, or CNS involvement, corticosteroids may also be needed. Treatment may not be effective in ocular larva migrans; corticosteroid injections may reduce inflammation, and surgery may be necessary to manage secondary damage.
Trichinosis
Mebendazole is used to treat trichinosis caused by Trichinella spiralis. Although some clinicians state that albendazole and mebendazole are equally effective for trichinosis, others consider mebendazole the drug of choice and albendazole an alternative, especially during the tissue phase of the illness. Adding corticosteroids to the anthelmintic is usually recommended, particularly when symptoms are severe. Corticosteroids help relieve the inflammatory reaction and can be lifesaving when the heart or CNS is involved.
Trichuriasis
Mebendazole is used to treat trichuriasis caused by Trichuris trichiura (whipworm). It is considered a drug of choice for this infection.
Other Nematode Infections
Mebendazole used together with corticosteroids appeared to shorten the course of infection, but not the number of relapses, in several patients with eosinophilic meningitis caused by Angiostrongylus cantonensis. No drug has been shown to be effective for this infection, and some patients have worsened when treated with albendazole, mebendazole, thiabendazole, or ivermectin. Mebendazole has also been used in animals to treat angiostrongyliasis caused by A. costaricensis or A. malaysiensis.
Mebendazole is considered the drug of choice, and albendazole is considered an alternative, for capillariasis caused by Capillaria philippinensis. Although metronidazole is generally considered the drug of choice for infections caused by Dracunculus medinensis (guinea worm) because it has been shown to reduce inflammation and help with removal of the worm, mebendazole (400-800 mg daily for 6 days) has been reported to kill the worm directly. Mebendazole is also used to treat infections caused by Trichostrongylus. Pyrantel pamoate is considered the drug of choice, and albendazole or mebendazole are alternatives, for Trichostrongylus infections. Mebendazole is considered a drug of choice for trichuriasis caused by Trichuris trichiura (whipworm).
Cestode (Tapeworm) Infections
Mebendazole has been used to treat intestinal infections caused by the adult forms of certain tapeworms, including Hymenolepis nana (dwarf tapeworm), Taenia saginata (beef tapeworm), and T. solium (pork tapeworm). However, other anthelmintics, usually praziquantel, are generally preferred for intestinal infections caused by the adult forms of these cestodes.
Mebendazole has been effective in a limited number of patients for the treatment of hydatid disease caused by the larval form of Echinococcus granulosus. However, albendazole is generally preferred to mebendazole, and surgery is considered the treatment of choice for hydatid disease when medically feasible. An anthelmintic may be given around the time of surgery in patients undergoing cyst removal to reduce the risk of dissemination during the procedure.
Mebendazole has also been used to treat alveolar hydatid disease caused by E. multilocularis in a very limited number of patients; however, surgical removal of the larval mass remains the recommended and most reliable treatment for these infections when feasible. Continuous albendazole or mebendazole therapy has reportedly been associated with clinical improvement in cases that cannot be surgically removed.
Giardiasis
Although metronidazole is generally the drug of choice for giardiasis caused by Giardia lamblia, mebendazole has been used in a limited number of adolescents and children.
Quick comparison: mebendazole vs alternatives
Dosage and Administration
Mebendazole is used to treat a variety of nematode (roundworm) infections, including trichuriasis (whipworm infection) caused by Trichuris trichiura, enterobiasis (pinworm infection) caused by Enterobius vermicularis, ascariasis (roundworm infection) caused by Ascaris lumbricoides, and hookworm infections caused by Ancylostoma duodenale, Necator americanus, or Ancylostoma caninum.
Administration
Mebendazole is taken by mouth. The tablets may be chewed, swallowed whole, or crushed and mixed with food. No special diet, fasting, or purgation is needed before taking the medicine. Patients should also be advised about hygiene measures to help reduce reinfection, such as wearing shoes, washing hands with soap and cleaning under the fingernails often during the day, especially before eating and after using the toilet, and washing all fruits and vegetables thoroughly before eating them.
Dosage
The dosage is the same for adults and children. The manufacturer states that if the patient is not cured 3 weeks after mebendazole therapy, a second course of treatment is advised.
Nematode (Roundworm) Infections: Ascariasis
For ascariasis caused by Ascaris lumbricoides, including mixed helminth infections, the usual mebendazole dosage for adults and children is 100 mg twice daily for 3 consecutive days. Alternatively, some clinicians suggest a single 500-mg dose for adults and children.
Enterobiasis
For enterobiasis caused by Enterobius vermicularis (pinworm) in adults and children, the usual mebendazole dose is 100 mg as a single dose. In addition, some clinicians recommend a second 100-mg dose 2 weeks later. The manufacturer states that if the patient is not cured within 3 weeks after the initial dose, a second dose should be given.
Filariasis
For filariasis caused by Mansonella perstans, some clinicians recommend mebendazole 100 mg twice daily for 30 days in adults and children. For onchocerciasis (filariasis caused by Onchocerca volvulus) in adults, a dosage of 1 g twice daily for 28 days has been suggested.
Hookworm Infections
For intestinal hookworm infections caused by Ancylostoma duodenale or Necator americanus, or for eosinophilic enterocolitis caused by Ancylostoma caninum (dog hookworm), the usual mebendazole dosage for adults and children is 100 mg twice daily for 3 consecutive days. Alternatively, some clinicians suggest a single 500-mg dose for adults and children with hookworm infections caused by A. duodenale or N. americanus.
Toxocariasis (Visceral Larva Migrans)
For toxocariasis (visceral larva migrans) caused by dog and cat roundworms, some clinicians recommend mebendazole 100 mg or 200 mg twice daily for 5 days in adults and children. However, the best treatment duration is not known, and some clinicians recommend continuing treatment for up to 20 days. A dosage of 1 g 3 times daily (50 mg/kg/day) for 21 days reportedly cured at least one patient with this infection.
Trichinosis
The recommended mebendazole dosage for trichinosis caused by Trichinella spiralis in adults and children is 200-400 mg 3 times daily for 3 days, followed by 400-500 mg 3 times daily for 10 days.
Trichuriasis
For trichuriasis caused by Trichuris trichiura (whipworm), adults and children should receive mebendazole 100 mg twice daily for 3 consecutive days. Alternatively, some clinicians suggest a single 500-mg dose for adults and children.
Other Nematode Infections
For capillariasis caused by Capillaria philippinensis, some clinicians recommend mebendazole 200 mg twice daily for 20 days in adults and children. For dracunculiasis caused by Dracunculus medinensis (guinea worm), a mebendazole dosage of 400-800 mg daily for 6 days has reportedly killed the worm directly. For infections caused by Trichostrongylus, adults and children should receive mebendazole 100 mg twice daily for 3 consecutive days.
Cautions
Adverse Effects
At the usual recommended dosages (that is, 100-200 mg daily), mebendazole appears to cause few side effects. Side effects seem to occur more often when higher doses are used, such as those used for extraintestinal infections like hydatid disease, and in some cases may be related to the drug killing the parasites. Temporary diarrhea and abdominal pain have occurred occasionally during mebendazole treatment, but these have usually been linked to very heavy infections and passage of the worms. Nausea, vomiting, headache, tinnitus, numbness, and dizziness have also been reported occasionally during mebendazole therapy.
Fever has occurred in some patients, especially those receiving high-dose treatment for extraintestinal infections. Bone marrow suppression, seen as neutropenia (including agranulocytosis) and/or thrombocytopenia, has also been reported in patients receiving high-dose mebendazole therapy (for example, 30-50 mg/kg/day) for extraintestinal infections. Although this usually reversed after the drug was stopped, death has rarely occurred. Other side effects reported rarely in patients receiving mebendazole include alopecia, rash, pruritus, urticaria, angioedema, flushing, hiccups, cough, weakness, drowsiness, chills, hypotension, seizures, temporary abnormalities in liver function tests (for example, increased serum aminotransferase, alkaline phosphatase, and/or bilirubin concentrations), increased BUN, decreased hemoglobin concentration and/or hematocrit, leukopenia, thrombocytopenia, eosinophilia, hematuria, and cylindruria. Migration of roundworms through the mouth and nose has also been reported.
Precautions and Contraindications
Mebendazole is contraindicated in patients who are hypersensitive to the drug.
Pediatric Precautions
In Canadian practice, the safety of mebendazole in children younger than 2 years of age has not been established. Because of limited experience with mebendazole in children younger than 2 years of age, the drug should be used in these children only when the potential benefits justify the possible risks.
Mutagenicity and Carcinogenicity
Animal and in vitro studies have not shown mebendazole to be mutagenic. No evidence of carcinogenesis was seen in rats and mice receiving mebendazole dosages up to 40 mg/kg/day for more than 2 years.
Pregnancy, Fertility, and Lactation
Mebendazole has been shown to be embryotoxic and teratogenic in rats when given as single oral doses as low as 10 mg/kg. Although there are no adequate and controlled studies in humans to date, the rate of spontaneous abortion and malformation did not exceed that of the general population in a limited number of women who inadvertently received the drug during the first trimester of pregnancy; no teratogenic risk associated with mebendazole therapy was identified in 170 full-term deliveries. Mebendazole should be used during pregnancy, especially during the first trimester, only when the potential benefits justify the possible risks to the fetus. If the drug is used during pregnancy, the patient should be informed of the potential risk to the fetus. Reproduction studies in male and female rats using mebendazole dosages up to 40 mg/kg for 60 days and 14 days prior to gestation, respectively, did not show evidence of impaired fertility; however, slight maternal toxicity occurred. Since it is not known whether mebendazole passes into breast milk, the drug should be used with caution in nursing women.
Drug Interactions
Anticonvulsants
Limited data suggest that both carbamazepine and phenytoin may increase the metabolism of mebendazole, likely by inducing hepatic microsomal enzymes, which lowers mebendazole levels in the blood. This interaction is unlikely to be clinically important in patients taking mebendazole to treat intestinal worm infections. However, carbamazepine or phenytoin may prevent an adequate treatment response in patients taking the anthelmintic for extraintestinal infections (for example, hydatid disease). Pending more data, alternative anticonvulsants (for example, valproic acid) should be considered in patients receiving mebendazole for extraintestinal infections.
Cimetidine
Preliminary evidence suggests that cimetidine inhibits mebendazole metabolism and may increase plasma concentrations of the drug.
Acute Toxicity
An overdose of mebendazole may cause GI symptoms that last for up to a few hours. If acute overdose occurs, vomiting and purging should be induced. Activated charcoal may be given.
Mechanism of Action
Although the exact way mebendazole works has not been fully established, the drug appears to selectively and irreversibly inhibit the uptake of glucose and other low-molecular-weight nutrients in susceptible helminths. Blocking glucose uptake appears to deplete the parasite's glycogen stores. Mebendazole does not inhibit glucose uptake in mammals.
Mebendazole appears to cause degenerative changes in the intestine of nematodes and in the absorptive cells of cestodes. The drug's main anthelmintic effect appears to be degeneration of cytoplasmic microtubules within these intestinal and absorptive cells. Deterioration of the microtubules inhibits organelle movement and interferes with absorptive and secretory function. As a result of excessive buildup of intracellular transport secretory granules, hydrolytic and proteolytic enzymes are released and cause cellular autolysis. This irreversible damage leads to death of the parasite.
Mebendazole has no effect on blood glucose levels in humans, and examination of the intestine and other organs of treated animals has shown an intact microtubular system and normal subcellular organelles. The presence of food in the digestive tract of the definitive host does not affect the drug's action during treatment of intestinal helminth infections.
Spectrum: Mebendazole is active against certain nematodes (roundworms) that infect humans, including Ancylostoma duodenale (hookworm), Angiostrongylus cantonensis, Ascaris lumbricoides (roundworm), Capillaria philippinensis (Philippine threadworm), Enterobius vermicularis (pinworm), Gnathostoma spinigerum, Necator americanus (hookworm), Strongyloides stercoralis (threadworm), Trichinella spiralis (pork worm), and Trichuris trichiura (whipworm). However, the drug's activity against S. stercoralis is variable and is usually lower than against other nematodes.
Mebendazole has been reported to be filaricidal against Mansonella perstans and Onchocerca volvulus. Mebendazole has also been shown to be active against certain cestodes (tapeworms), including Hymenolepis nana (dwarf tapeworm), Taenia saginata (beef tapeworm), T. solium (pork tapeworm), and Echinococcus granulosus (hydatid cyst).
Pharmacokinetics
Absorption
Mebendazole appears to be minimally absorbed from the GI tract after oral administration. Limited data indicate that about 2-10% of an oral dose is absorbed. Peak plasma concentrations of mebendazole occur about 0.5-7 hours after oral administration and vary widely between patients. After multiple oral doses of mebendazole (40 mg/kg/day) in 2 adults with hydatid cysts, mean peak plasma concentrations of about 0.08 mcg/mL occurred at 0.5-2 hours. Following oral administration of a single 10-mg/kg dose of mebendazole to patients with hydatid cysts in another study, peak plasma concentrations were low and occurred at about 1.5-7 hours. Following oral administration of multiple doses of mebendazole (100 mg twice daily for 3 days) to several children, peak plasma mebendazole concentrations did not exceed 0.03 mcg/mL, and peak plasma concentrations of the 2-amino metabolite of the drug, the major metabolite, did not exceed 0.09 mcg/mL.
Distribution
Mebendazole is highly bound to plasma proteins. It is not known whether mebendazole is distributed into breast milk.
Elimination
The elimination half-life of mebendazole has been reported to be about 2.8-9 hours. Although the exact metabolic fate of mebendazole has not been fully determined, the drug is metabolized by decarboxylation to 2-amino-5(6)-benzimidazolyl phenylketone; this metabolite does not have anthelmintic activity. About 2-10% of an oral dose of mebendazole is excreted in the urine within 24-48 hours of administration, mainly as unchanged drug and the 2-amino metabolite. The metabolic fate and excretion rate of unabsorbed mebendazole have not been determined.
Chemistry and Stability
Chemistry
Mebendazole is a synthetic benzimidazole-derivative anthelmintic agent. The drug is structurally related to albendazole and thiabendazole. Mebendazole is a white to slightly yellow powder and is practically insoluble in water and alcohol.
Stability
Commercially available mebendazole chewable tablets should be stored at 15-25°C in tightly closed containers and have an expiry date of 3 years from the date of manufacture.
Organs and Systems
Liver
All benzimidazoles can cause mild, reversible increases in transaminases, but even at high doses stopping treatment is justified in only a few patients.
Granulomatous hepatitis with eosinophilia has been attributed to mebendazole.
A 52-year-old man with ascariasis took two 3-day courses of mebendazole 100 mg twice daily, with a 2-week interval. Within 48 hours of the second course, he developed fever (39°C), diarrhea, anorexia, and prostration. Ten days later, he had tender hepatomegaly. His liver function tests were abnormal (aspartate transaminase 466 IU/1, alanine transaminase 458 IU/1). Serum alkaline phosphatase and bilirubin were normal, and gamma-glutamyl transferase was mildly elevated. The white blood cell count was 12.7 x 109/1 with 18% eosinophils.
Coagulation was normal. Tests for hepatitis A, B, and C, cytomegalovirus, and Epstein-Barr virus were all negative. Serum ACE was not elevated. Antimitochondrial antibodies were negative, but antinuclear antibodies and antibodies against smooth muscle were positive. Extensive testing to rule out other causes of granulomatous hepatitis was negative. A liver biopsy showed multiple granulomata consisting of epithelioid cells, multinucleated giant cells, plasma cells, and lymphocytes.
There was slight fibrosis around the granulomata. There was no evidence of cholestasis. No helminth ova were found. Ziehl-Nielsen and periodic acid Schiff stains were both negative. After 2 days, the fever had settled without treatment and he felt better. Serum transaminases returned to normal over the next 10 weeks, and the eosinophilia disappeared.
Liver damage has been described after treatment with most benzimidazoles, but it is usually cholestatic. The liver damage described in this case was granulomatous. Liver damage after mebendazole at the low dose used in this case is rare, probably because of poor absorption.
It is more common, although still rare, at the higher doses used to treat human echinococcosis.
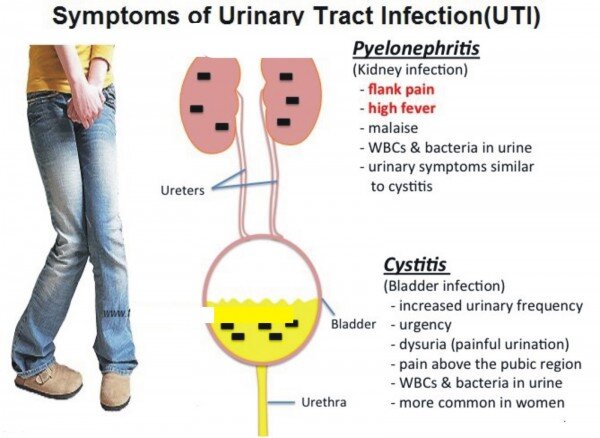
Urinary tract
Glomerulonephritis has been observed in five patients from Kenya.
Skin
Two cases of exfoliative dermatitis occurred among a total of 131 treated patients. In one case from India, a fixed drug eruption was attributed to the drug, and other types of rash have also been reported.
An outbreak of Stevens-Johnson syndrome has been reported in 52 Filipino overseas contract workers (aged 20-30 years, 50 women) working in China who used mebendazole for helminth prophylaxis. All took mebendazole at least once after the appearance of rash and fever. Three women eventually died, mainly due to septicemia.
Side Effects
Mebendazole, a benzimidazole, is poorly absorbed from the gut, although it reliably enters cyst fluid. It is therefore most useful for treating intestinal infections and cyst-forming infestations. It is mainly an anthelmintic drug and is effective against hookworm, ascariasis, enterobiasis, and trichuriasis. Mebendazole is effective against enteric Strongyloides, but because it is not absorbed it is ineffective against tissue forms. However, it is also effective against Giardia lamblia, while Trichomonas vaginalis is susceptible in vitro. Mebendazole does not interfere with the normal intestinal flora.
Mebendazole has been studied across a range of doses and treatment durations. The most common dose is 100 mg twice daily for 3 days. Absorption is minimal, but plasma concentrations vary considerably; the half-life is 2-9 hours. Much higher doses, up to 60 mg/kg/day, have been used in inoperable cases of cystic echinococcosis, and unwanted effects are then more common.
Flubendazole is an analogue of mebendazole used in intestinal helminthiasis and hydatid disease. In trials of two-dose oral treatment for intestinal helminthiasis, reactions were mild and uncommon. They included nausea, abdominal pain, dyspepsia, and sleepiness. Later field experience has not suggested that flubendazole differs appreciably from other drugs in this class in terms of side effects.
Comparative studies
Echinococcosis
The use of albendazole and mebendazole in patients with hydatid disease has been evaluated in a large number of patients with Echinococcus granulosus hydatid cysts. In these reports, continuous treatment with albendazole or mebendazole produced degenerative changes in many cysts, with albendazole generally showing greater activity than mebendazole. During long-term follow-up, some cysts relapsed, often within the first 2 years, and additional treatment with albendazole was effective in many relapsed cases. Current guidance generally considers albendazole the preferred benzimidazole for cystic echinococcosis, while mebendazole is usually regarded as an alternative.
Side effects during the first treatment period consisted of increased transaminases with albendazole (67 of 323 patients) and mebendazole (16 of 125 patients), and abdominal pain in 12% and 11%, respectively. With both drugs, some patients also experienced headache, abdominal distension, vertigo, urticaria, jaundice, thrombocytopenia, fever, or dyspepsia, but most of these are known manifestations of echinococcus infection. Six of 323 patients taking albendazole stopped treatment because of side effects, compared with eight of 125 patients taking mebendazole. Albendazole appears to be more effective than mebendazole in the treatment of hydatid cysts caused by E. granulosis, and the intensity and frequency of the usually mild side effects appear to be similar with both drugs.
In 78 patients with hydatid disease, there was a low recurrence rate (below 3%) after a postoperative prophylactic course of mebendazole 20 mg/kg/day in three divided doses for 3 months. The only side effect of mebendazole was excessive hair loss in two women. The unusually low recurrence rate of hydatid disease after treatment with mebendazole in this study was later questioned and attributed to meticulous surgical technique, with avoidance of hydatid fluid spillage and complete removal of parasitic components.
General adverse effects
At normal doses (100 mg twice daily for 3 days), mild headache, dizziness, and nausea or diarrhea are common; allergic reactions can also occur. Mild and reversible increases in transaminases can occur and should be monitored, but even at high doses stopping treatment is justified in only a few patients. Neutropenia has been reported and can be severe and persistent. High doses (up to 50-60 mg/kg) can also cause alopecia and cough. Mebendazole has been associated with extra-intestinal migration of Ascaris in heavily infected patients. Apart from the poor treatment response seen in about 25% of cases, drug toxicity, especially with high prolonged doses, has led to treatment withdrawal in a small proportion of patients.
Side effects severe enough to lead to withdrawal have included worsening of pre-existing hyperlipidemia (type IV), progressive uremia, and a marked rise in liver enzymes. One person developed a rash accompanied by a striking rise in serum transaminases, which recurred on later re-exposure. Experience in the treatment of Echinococcus multilocularis infection is similar. One patient with fatal agranulocytosis also had severe, probably unrelated, liver disease. About 3-4% develop fever, which can be persistent and accompanied by respiratory symptoms and eosinophilia. Other side effects include pain over the site of the cyst, allergic reactions, alopecia, glomerulonephritis, and rashes.
Various authors have reported spontaneous rupture of hydatid cysts with mebendazole, and this is probably more frequent than in untreated individuals. Pleural and peritoneal cysts are more likely to rupture.
Evidence of teratogenicity in rats has not been accompanied by reports of harm in human pregnancy, but the World Health Organization (WHO) recommends avoiding it during the first trimester. It is not known whether mebendazole passes into breast milk; no side effects have been reported, but this has not been specifically studied.
Mebendazole: Organs and Systems
Susceptibility Factors
Age
Children under 2 years of age with helminth infections are currently excluded from treatment with mebendazole and other anthelmintic drugs based on the manufacturer's instructions. In a double-blind, randomized trial in Tanzania, 212 children under 2 years of age were given a total of 653 anthelmintic treatments (317 mebendazole 500 mg; 336 placebo). There were no significant differences in adverse events between the two groups. In light of the potential nutritional benefit of regular deworming in this age group, the policy excluding children under 2 years of age from treatment should probably be reconsidered.
Storage
Store at room temperature 20-25°C (68-77°F). Keep in the original container, tightly closed, away from moisture and direct sunlight. Keep out of reach of children.