Ciloxan Ophthalmic Solution (Ciprofloxacin)

Dosages
Ciloxan Ophthalmic Solution 5 ml
| Quantity | Price per bottle | Total price | |
|---|---|---|---|
| 4 | C$17.30 | C$69.21 | |
| 5 | C$15.78 | C$78.89 | |
| 6 | C$14.53 | C$87.20 |
Payment & Shipping
Your order is carefully packed and ships within 24 hours. Here is what a typical package looks like.
Sized like a regular personal letter (approximately 24x11x0.7 cm), with no indication of what is inside.



| Shipping Method | Estimated delivery |
|---|---|
| Express Free for orders over C$415.23 | Estimated delivery to Canada: 4-7 days |
| Standard Free for orders over C$276.82 | Estimated delivery to Canada: 14-21 days |








Discount Coupons
- Canada Day - July 1, 2026 10% CANADADAY10
- Boxing Day - December 26, 2026 12% BOXING12
Brand Names
| Country | Brand Names |
|---|---|
 Colombia Colombia | Alcon Cilox |
 Hong Kong Hong Kong | CiprocIN |
 Indonesia Indonesia | Alcon Cilox Baquinor |
 Malaysia Malaysia | Ciflox |
 Portugal Portugal | Oftacilox |
 Spain Spain | Oftacilox |
Description
Ciprofloxacin is generally well tolerated, and its side effects are similar to those reported with other quinolone anti-infectives (for example, norfloxacin and ofloxacin). Side effects have been reported in 5-14% of patients taking ciprofloxacin and were severe enough to require stopping treatment in 2-3.5% of patients. The most common side effects affect the gastrointestinal (GI) tract or central nervous system (CNS), and the effects that led to stopping treatment mainly involved these body systems as well.
There is currently limited information on side effects of ciprofloxacin in people receiving post-exposure prophylaxis for anthrax. In response to a questionnaire given to 490 such individuals in Florida at about day 7 or 14 of anti-infective prophylaxis, 19% sought medical attention for an anti-infective-related side effect or reported one or more of the following: itching, breathing problems, or swelling of the face, neck, or throat.
Although the percentage of patients in this subgroup who received ciprofloxacin versus other anti-infectives was not reported, 86% of all patients (whether or not they answered the questionnaire) received ciprofloxacin, and 80% continued prophylaxis beyond 14 days. In an epidemiologic evaluation of 8424 postal workers who were offered 60 days of anthrax prophylaxis and given a questionnaire in New Jersey, New York City, and the District of Columbia on days 7-10 of anti-infective prophylaxis, 5819 completed or were given the questionnaire, and 3863 of them had started prophylaxis (3428 with ciprofloxacin).
Among those treated with ciprofloxacin, 19% reported severe nausea, vomiting, diarrhea, and/or abdominal pain; 14% reported fainting, light-headedness, and/or dizziness; 7% reported heartburn or acid reflux; 6% reported rash, urticaria, and/or itching; and 8% stopped treatment with the drug (3% because of side effects, 1% because of fear of developing a side effect, and 1% because they were confused about the need for treatment). Only 2% of those taking any anti-infective sought medical attention for possible signs of anaphylaxis, and none required hospitalization.
GI Effects
Nausea, diarrhea, vomiting, and abdominal pain or discomfort have been reported in 2-10% of patients receiving ciprofloxacin. These effects are generally mild and temporary and occur most often in older adults and/or when high doses are used. Loss of appetite, dyspepsia, flatulence, GI erosion and bleeding, dysphagia, bad taste, intestinal perforation, painful oral mucosa, and oral candidiasis have been reported in less than 1% of patients receiving the drug.
Effects on Fecal Flora
Ciprofloxacin has a selective effect on normal bowel flora. Although fluoroquinolones, including ciprofloxacin, are relatively inactive against Clostridium difficile in vitro, C. difficile-associated diarrhea and colitis (also known as antibiotic-associated pseudomembranous colitis) have been reported in 1% or less of patients receiving these drugs. In addition, C. difficile-associated diarrhea and colitis caused by other anti-infectives (for example, ceftriaxone) have resolved in several patients after those other anti-infectives were stopped and ciprofloxacin was started.
The reason for this relatively weak association between ciprofloxacin and colitis has not been established, but it may be related to fecal concentrations of the drug that greatly exceed the minimum inhibitory concentration (MIC) of C. difficile and/or to the selective effect of the drug on normal GI flora. It should be noted, however, that starting ciprofloxacin in these patients may not have been responsible for the colitis resolving and may simply have allowed it to improve after the offending anti-infective was discontinued.
The possibility that diarrhea developing in any patient treated with ciprofloxacin may be secondary to C. difficile-associated colitis should be considered. C. difficile-associated diarrhea and colitis can range from mild to life-threatening. Mild cases of colitis may respond to stopping ciprofloxacin alone, but diagnosing and managing moderate to severe cases should include appropriate bacteriologic studies and treatment with fluid, electrolyte, and protein replacement as needed. If colitis is moderate to severe or does not improve after ciprofloxacin is discontinued, appropriate anti-infective treatment (for example, oral metronidazole or vancomycin) should be given. Isolation of the patient may be advisable. Other causes of colitis should also be considered.
Total bacterial counts of normal anaerobic fecal flora are generally unaffected during or after ciprofloxacin therapy. However, total bacterial counts of normal aerobic fecal flora decrease within 2-5 days after treatment with the drug is started and generally return to pretreatment levels within 1-4 weeks after the drug is discontinued. Ciprofloxacin therapy generally greatly reduces or completely eradicates normal fecal Enterobacteriaceae; the drug reduces fecal aerobic gram-positive bacteria to a lesser extent. Ciprofloxacin therapy does not appear to affect total bacterial counts of normal salivary flora, including streptococci, staphylococci, and anaerobic bacteria.
Nervous System Effects
Headache and restlessness have been reported in about 1-2% of patients receiving ciprofloxacin. Dizziness, light-headedness, insomnia, nightmares, hallucinations, manic reaction, toxic psychosis, irritability, tremor, ataxia, seizures, lethargy, drowsiness, vertigo, anxiety, nervousness, confusion, weakness, malaise, phobia, depersonalization, depression, suicidal thoughts or acts, paresthesia, and increased intracranial pressure have been reported in less than 1% of patients. Some of these reactions may occur after the first dose. If seizures or other severe CNS reactions occur during ciprofloxacin therapy, the drug should be discontinued and appropriate measures started.
Some CNS side effects may be related to the fact that ciprofloxacin, like other fluoroquinolones, is a gamma-aminobutyric acid (GABA) inhibitor. In addition, it has been suggested that some CNS stimulant effects reported in patients receiving the drug may result from ciprofloxacin-induced changes in caffeine pharmacokinetics.
Dermatologic and Sensitivity Reactions
Mild, temporary rash has been reported in 1-4% of patients, and eosinophilia, itching, urticaria, cutaneous candidiasis, hyperpigmentation, erythema nodosum, angioedema, and swelling of the face, neck, lips, conjunctivae, or hands have been reported in less than 1%. Flushing, fever, chills, and photosensitivity have also been reported in less than 1% of patients receiving the drug. Severe hypersensitivity reactions characterized by rash, fever, eosinophilia, jaundice, and hepatic necrosis (including fatal cases) have rarely been reported in patients receiving ciprofloxacin together with other drugs.
Toxic epidermal necrolysis has been reported rarely in patients receiving ciprofloxacin. Therefore, the manufacturer recommends that ciprofloxacin be discontinued at the first sign of rash or any other sign of hypersensitivity. In addition, serious and occasionally fatal hypersensitivity (anaphylactic and anaphylactoid) reactions have occurred, some with the initial dose, in patients receiving quinolone therapy. Some reactions were accompanied by cardiovascular collapse, loss of consciousness, paresthesia, pharyngeal or facial edema, dyspnea, urticaria, and/or itching; a history of hypersensitivity was present in only a few cases.
Limited evidence suggests that the frequency of severe hypersensitivity reactions may be higher in patients with acquired immunodeficiency syndrome (AIDS) than in other patients, although the exact mechanism for this increased risk has not been determined. If a severe hypersensitivity reaction occurs during ciprofloxacin therapy, the drug should be discontinued and the patient given appropriate treatment (for example, epinephrine, corticosteroids, maintenance of an adequate airway, oxygen, and maintenance of blood pressure) as indicated.
Genitourinary Effects
Increased serum creatinine and blood urea nitrogen (BUN) concentrations have occurred in about 1% of patients receiving ciprofloxacin. Interstitial nephritis, nephritis, renal failure, dysuria, polyuria, urinary retention, albuminuria, urethral bleeding, vaginitis, and acidosis have been reported in less than 1% of patients. In at least one patient, acute renal failure associated with interstitial nephritis occurred within about 2 weeks after starting ciprofloxacin and appeared to be a hypersensitivity reaction; renal biopsy showed marked interstitial edema with extensive lymphocytic infiltrations and occasional eosinophils. Crystalluria, cylindruria, and hematuria have been reported rarely.
Crystalluria generally occurs in patients with alkaline urine who receive high doses and has not been associated with changes in renal function. The risk of crystal formation and crystalluria in patients receiving the usual recommended doses (250-750 mg) is low if urine pH is within the usual range (that is, less than 6.8). Patients taking the drug, particularly at relatively high doses, should maintain adequate fluid intake; in addition, alkaline urine should be avoided.
Musculoskeletal Effects
Arthralgia, joint or back pain, joint inflammation, joint stiffness, achiness, vasculitis, neck or chest pain, and flare-up of gout have been reported in less than 1% of patients. Achilles and other tendon ruptures that required surgical repair or resulted in prolonged disability have been reported in patients receiving fluoroquinolones, including ciprofloxacin.
Ciprofloxacin should be discontinued in any patient who experiences tendon pain, inflammation, or rupture. Ciprofloxacin, like most other fluoroquinolones, causes arthropathy in immature animals of various species. Ciprofloxacin has caused damage to weight-bearing joints in juvenile dogs and rats. In young beagles, ciprofloxacin 100 mg/kg for 4 weeks caused degenerative articular changes of the knee joint; at 30 mg/kg/day, effects were minimal, although some damage to weight-bearing joints was observed even at the lower dose. Removing weight-bearing from the joint reduced the lesions but did not completely prevent them.
Morphologic changes observed in animals with quinolone-induced arthropathies include erosions in joint cartilage accompanied by noninflammatory, cell-free effusion of the joint space; the cartilage is incapable of regeneration and may serve as a site for the development of arthropathy deformans. In addition, breakdown products of cartilage may irritate the synovia. The relationship between these effects in animals and the rheumatologic symptoms associated with ciprofloxacin use in humans is unknown.
Hepatic Effects
Increased serum concentrations of aspartate aminotransferase (AST; formerly SGOT) and alanine aminotransferase (ALT; formerly SGPT) have been reported in about 2% of patients. Increased serum concentrations of alkaline phosphatase, lactate dehydrogenase (LDH), bilirubin, and gamma-glutamyltransferase (GGT; also called GGTP) have been reported in less than 1%. Fulminant and occasionally fatal hepatic failure has occurred rarely in patients receiving ciprofloxacin.
Hematologic Effects
Eosinophilia, leukopenia, neutropenia, increased or decreased platelet count, and pancytopenia have been reported in less than 1% of patients. Anemia, decreased hemoglobin, increased monocytes, leukocytosis, and bleeding diathesis have been reported in less than 1%. Transient acquired von Willebrand disease has been reported rarely; factor VIII concentration returned to normal values several months (that is, 5-6 months) after the drug was discontinued.
Cardiovascular Effects
Palpitation, atrial flutter, ventricular ectopy, syncope, hypertension, angina pectoris, chest pain, myocardial infarction, cardiopulmonary arrest, and cerebral thrombosis have been reported in less than 1% of patients.
Local Effects
Local side effects have been reported at the infusion site following IV administration of ciprofloxacin. These reactions generally resolve quickly after the infusion is completed and have been reported most often when IV infusions were given over 30 minutes or less. The manufacturer states that local side effects do not rule out later IV administration unless the reactions recur or worsen.
Other Adverse Effects
Epistaxis, laryngeal or pulmonary edema, hiccups, hemoptysis, dyspnea, bronchospasm, and pulmonary embolism have been reported in less than 1% of patients. Blurred vision, disturbed vision (for example, change in colour perception, excessive brightness of lights), decreased visual acuity, diplopia, and eye pain have been reported in less than 1% of patients receiving ciprofloxacin. Tinnitus, anosmia, increased serum amylase, decreased blood glucose, and increased serum uric acid concentrations have been reported rarely (that is, in less than 0.1% of patients).
Precautions and Contraindications
Crystalluria has been reported rarely. Although crystalluria is not expected under usual conditions and at the usual recommended doses, patients should be instructed to drink enough fluids to maintain proper hydration and adequate urine output during ciprofloxacin therapy. Measures should also be taken to avoid alkaline urine, and the recommended dose should not be exceeded.
Because ciprofloxacin may stimulate the CNS and could potentially result in tremor, restlessness, light-headedness, mental confusion, toxic psychosis, and/or seizures, the drug should be used with caution in patients with known or suspected CNS disorders (for example, severe cerebral arteriosclerosis, seizure disorders) that predispose them to seizures or lower the seizure threshold, and when other factors are present (for example, certain drug therapies, renal dysfunction) that also predispose to seizures or lower the seizure threshold. Patients should be advised that ciprofloxacin may cause dizziness or light-headedness, and their individual response should be known before driving or operating machinery or doing activities that require mental alertness and coordination.
Patients receiving a theophylline derivative or caffeine at the same time may also be at increased risk of these CNS effects. Serious and fatal reactions, including cardiac arrest, seizures, status epilepticus, and respiratory failure, have been reported during concurrent theophylline and ciprofloxacin therapy. Patients should be advised to stop the drug and tell their physician if they experience tendon pain, inflammation, or rupture, and to rest and avoid exercise.
As with other anti-infectives, ciprofloxacin may result in overgrowth of nonsusceptible organisms, especially enterococci or Candida. Resistant strains of some organisms (for example, Pseudomonas aeruginosa, staphylococci) have developed during ciprofloxacin therapy. Careful monitoring of the patient and periodic in vitro susceptibility testing are essential. If superinfection occurs, appropriate treatment should be started. In Canadian clinical practice, the dose and/or frequency of IV ciprofloxacin, conventional tablets, or oral suspension should be reduced in patients with severe renal impairment because serum concentrations are higher and last longer than in patients with normal renal function.
The manufacturer recommends that organ system function, including renal, hepatic, and hematopoietic function, be monitored periodically during prolonged ciprofloxacin therapy. Patients should be advised to avoid excessive exposure to sunlight or artificial ultraviolet light and to stop therapy if phototoxicity occurs. Moderate to severe phototoxicity, appearing as an exaggerated sunburn reaction, has been reported during exposure to direct sunlight in patients receiving some fluoroquinolones (for example, lomefloxacin, ofloxacin, sparfloxacin).
Ciprofloxacin can cause serious, potentially fatal hypersensitivity reactions, sometimes after the first dose. Patients should be advised of this possibility and instructed to stop the drug and contact their physician at the first sign of rash or any other sign of hypersensitivity. Ciprofloxacin is contraindicated in patients with a history of hypersensitivity to the drug or to other quinolones.
Pediatric Precautions
Anthrax
Ciprofloxacin may be used in children for inhalational anthrax (post-exposure) to reduce the incidence or progression of disease following exposure to aerosolized Bacillus anthracis spores. In Canada, public health guidance and expert recommendations generally support initial treatment of inhalational or systemic anthrax (including GI and oropharyngeal disease) with either IV ciprofloxacin or doxycycline plus 1 or 2 additional anti-infectives. Because of the potential side effects from prolonged ciprofloxacin use in infants and children, amoxicillin may be used to complete the remaining 60 days of therapy when penicillin susceptibility is known; amoxicillin is not recommended for initial treatment. Amoxicillin may also be considered as an alternative to ciprofloxacin for post-exposure prophylaxis when there are concerns about prolonged quinolone therapy in children.
Other Infections
Because ciprofloxacin causes arthropathy in immature animals, the manufacturer states that safety and effectiveness for other indications in children and adolescents younger than 18 years of age have not been established. Some clinicians suggest quinolones may be used cautiously in adolescents if skeletal growth is complete and that the potential benefits may outweigh the possible risks in certain children 9-18 years of age with serious infections (for example, cystic fibrosis, typhoid fever) when the causative organism is resistant to other available anti-infectives.
In Canadian practice, use of fluoroquinolones (for example, ciprofloxacin, levofloxacin, lomefloxacin, norfloxacin, ofloxacin, sparfloxacin) in children younger than 18 years of age may be justified in special circumstances; however, these drugs should be used only after careful assessment of the risks and benefits for the individual patient and after these have been explained to parents or caregivers.
Ciprofloxacin has been used in children with cystic fibrosis, but transient arthropathy has occasionally occurred. In at least one 16-year-old, arthropathy was associated with relatively high doses (750 mg twice daily) for several weeks. Ciprofloxacin has also been used in a limited number of children with typhoid fever resistant to other anti-infectives (for example, ampicillin, amoxicillin, chloramphenicol, co-trimoxazole). Short-term safety data are available from a randomized, double-blind study in children and adolescents 5-17 years of age with cystic fibrosis who received IV ciprofloxacin for acute pulmonary exacerbations.
Patients received IV ciprofloxacin (10 mg/kg every 8 hours) for 1 week followed by oral ciprofloxacin (20 mg/kg every 12 hours) to complete 10-21 days of therapy, or IV ceftazidime (50 mg/kg every 8 hours) plus IV tobramycin (3 mg/kg every 8 hours) for 10-21 days. Safety was monitored by periodic range-of-motion examinations and gait assessments; patients were followed for an average of 23 days after completion of therapy (range: 0-93 days). Local reactions at the injection site were reported more frequently with ciprofloxacin (24%) than with ceftazidime/tobramycin (8%), but other side effects were similar. In the ciprofloxacin group, musculoskeletal side effects, decreased range of motion, and arthralgia were reported in 22%, 12%, and 10%, respectively; in the combination group, these effects were 21%, 16%, and 11%.
One pediatric patient developed arthritis of the knee 9 days after a 10-day course of ciprofloxacin; clinical symptoms resolved, but magnetic resonance imaging (MRI) showed knee effusion without other abnormalities 8 months after treatment. A causal relationship could not be established, particularly since patients with cystic fibrosis may develop arthralgia and/or arthritis as part of the underlying disease process.
Geriatric Precautions
Retrospective analysis of 23 multiple-dose controlled clinical studies evaluating ciprofloxacin in more than 3500 patients showed that 25% were 65 years of age or older and 10% were 75 years of age or older. Although no overall differences in safety or effectiveness were observed between older adults and younger adults, the possibility that some older patients may be more sensitive cannot be ruled out. Ciprofloxacin is substantially eliminated by the kidney, and the risk of side effects may be greater in patients with impaired renal function. Although the dose does not need to be changed in individuals older than 65 years of age with normal renal function, the greater frequency of reduced renal function in older adults should be considered and the dose selected carefully; monitoring renal function may be helpful.
Mutagenicity and Carcinogenicity
Ciprofloxacin was not mutagenic in the rat hepatocyte DNA repair assay or in dominant lethal or micronucleus tests in mice. Ciprofloxacin tested positive for mutagenicity in the mouse lymphoma cell forward mutation assay and rat hepatocyte DNA repair assay; however, it was not mutagenic in other in vitro studies, including the Ames microbial (Salmonella) mutagen test with metabolic activation, Escherichia coli DNA repair assay, Chinese hamster V-79 cell HGPRT test, Syrian hamster embryo cell transformation assay, Saccharomyces cerevisiae point mutation assay, and mitotic crossover and gene conversion assays. No evidence of carcinogenic or tumour-forming potential was seen in mice or rats given oral ciprofloxacin 700 mg/kg daily or 250 mg/kg daily, respectively, for up to 2 years.
Pregnancy, Fertility and Lactation
There are currently no adequate, controlled studies of ciprofloxacin use in pregnant women. Because this drug, like most other fluoroquinolones, causes arthropathy in immature animals, ciprofloxacin should not be used during pregnancy except for the treatment or prevention of inhalational anthrax.
Reproduction studies in rats and mice using ciprofloxacin doses up to 6 times the usual human dose have not shown evidence of reduced fertility or harm to the fetus. In rabbits, ciprofloxacin 30 and 100 mg/kg caused adverse GI effects that led to maternal weight loss and a higher rate of abortion, but there was no evidence of teratogenicity. IV ciprofloxacin in rabbits at doses up to 20 mg/kg did not result in maternal toxicity, embryotoxicity, or teratogenicity.
Ciprofloxacin is excreted into human milk. Because of the potential for serious adverse reactions in breastfed infants, the Canadian product monograph states that a decision should be made to either discontinue breastfeeding or discontinue the drug, taking into account the importance of the medication to the woman. However, published references also note that infant exposure through breast milk is low, and some sources consider ciprofloxacin compatible with breastfeeding in certain situations. If prolonged therapy is required, the risks and benefits should be discussed with a healthcare professional.
Ciprofloxacin Hydrochloride: Drug Interactions
Antacids
Antacids containing magnesium, aluminum, or calcium decrease absorption of oral ciprofloxacin, resulting in lower serum and urine concentrations. Serum ciprofloxacin concentrations are generally decreased by 14-50%, but may be decreased by as much as 90% in patients taking an antacid at the same time; treatment failure may occur because of reduced absorption.
The mechanism has not been fully clarified, but magnesium, aluminum, and other divalent ions may bind to quinolones in the GI tract and form insoluble complexes. The manufacturer states that ciprofloxacin extended-release tablets, conventional tablets, or oral suspension should be taken at least 2 hours before or 6 hours after antacids containing magnesium or aluminum.
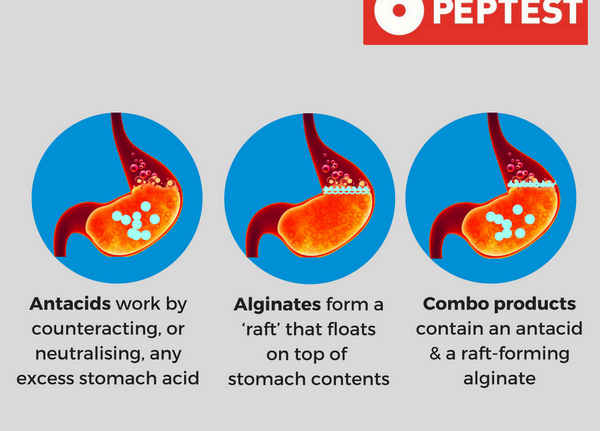
Some clinicians suggest telling patients not to take antacids containing magnesium, aluminum, or calcium at the same time as ciprofloxacin, or within 2-4 hours of a ciprofloxacin dose; however, others state that these antacids should not be used in patients receiving ciprofloxacin and that ciprofloxacin probably should not be used in patients with renal failure who require aluminum hydroxide or aluminum carbonate for intestinal binding of phosphate.
Aminoglycosides
The antibacterial activities of ciprofloxacin and aminoglycosides have been additive or synergistic in vitro against some strains of Enterobacteriaceae and Pseudomonas aeruginosa. However, synergism is unpredictable, and indifference generally occurs when ciprofloxacin is used with amikacin, gentamicin, or tobramycin against P. aeruginosa or Enterobacteriaceae. Indifference also generally occurs when ciprofloxacin is used with tobramycin against Acinetobacter.
Beta-Lactam Antibiotics
An additive or synergistic effect has occasionally occurred in vitro against some strains of P. aeruginosa and Stenotrophomonas maltophilia (formerly Pseudomonas maltophilia) when ciprofloxacin was used with an extended-spectrum penicillin (for example, mezlocillin, piperacillin). Indifference generally occurs when ciprofloxacin is used with an extended-spectrum penicillin against Enterobacteriaceae. Ciprofloxacin used with imipenem, cefoxitin, or a cephalosporin (for example, cefotaxime, ceftazidime, ceftizoxime) has been reported to be additive or synergistic against some strains of P. aeruginosa or Enterobacteriaceae; however, these combinations are generally indifferent rather than additive or synergistic. Ciprofloxacin with cefotaxime has shown synergistic activity in vitro against many strains of Bacteroides fragilis; antagonism did not occur.
Didanosine
Taking oral ciprofloxacin at the same time as didanosine given as chewable/dispersible buffered tablets or pediatric powder for oral solution (mixed with antacid) may decrease absorption of ciprofloxacin, resulting in lower serum and urine concentrations. The manufacturer states that ciprofloxacin extended-release tablets, conventional tablets, or oral suspension should be taken at least 2 hours before or 6 hours after these didanosine preparations.
Other Anti-infectives
The combination of ciprofloxacin and clindamycin has been synergistic in vitro against many strains of Peptostreptococcus, Lactobacillus, and B. fragilis. Synergism does not occur in vitro when ciprofloxacin is used with vancomycin against Staphylococcus epidermidis, S. aureus (including oxacillin-resistant strains), Corynebacterium, or Listeria monocytogenes. In vitro, the combination of ciprofloxacin and rifampin is generally indifferent against S. aureus; antagonism has been reported rarely.
Probenecid
Probenecid interferes with renal tubular secretion of ciprofloxacin, resulting in a 50% decrease in renal clearance, a 50% increase in systemic ciprofloxacin concentrations, and a longer serum half-life. This effect should be taken into account in patients receiving the drugs at the same time.
Cimetidine, Ranitidine, and Sucralfate
Sucralfate (presumably because of its aluminum content) decreases GI absorption of ciprofloxacin and may result in a substantial (for example, 50%) decrease in serum concentrations. Patients should be told to take ciprofloxacin extended-release tablets, conventional tablets, or oral suspension at least 2 hours before or 6 hours after sucralfate. Taking cimetidine or ranitidine at the same time does not appear to alter GI absorption of ciprofloxacin.
Coumarin Anticoagulants
Starting oral ciprofloxacin therapy in at least one patient stabilized on warfarin has resulted in prolongation of prothrombin time and hematemesis. Using other fluoroquinolones (for example, norfloxacin) at the same time in patients receiving coumarin anticoagulants has also resulted in increased prothrombin times. The mechanism has not been determined, but ciprofloxacin may displace anticoagulants from serum albumin binding sites. Ciprofloxacin should be used with caution in patients receiving a coumarin anticoagulant.
Iron, Multivitamins, and Mineral Supplements
Oral multivitamin and mineral supplements containing divalent or trivalent cations such as calcium, iron, or zinc may interfere with oral absorption of ciprofloxacin, resulting in lower serum and urine concentrations. These supplements should not be taken at the same time as ciprofloxacin. The manufacturer states that ciprofloxacin extended-release tablets, conventional tablets, or oral suspension should be taken at least 2 hours before or 6 hours after products containing calcium, iron, or zinc.
Xanthine Derivatives
Giving ciprofloxacin at the same time to patients receiving a theophylline derivative may result in higher and more prolonged serum theophylline concentrations and may increase the risk of theophylline-related side effects. Serum theophylline concentrations have reportedly increased by 17-254% and theophylline clearance decreased by 18-112% following initiation of ciprofloxacin; on average, clearance reductions have been about 20-35%.
Serious and fatal reactions have occurred during concomitant theophylline and ciprofloxacin therapy. If concomitant use is unavoidable, plasma theophylline concentrations should be monitored, the patient should be observed for toxicity, and the dose adjusted as needed. The need for dose adjustment should also be considered when ciprofloxacin is discontinued.
Although the clinical importance has not been determined, ciprofloxacin prolongs caffeine elimination half-life and decreases its volume of distribution and total body clearance. Patients should be advised that consuming large amounts of coffee, tea, caffeinated soft drinks, or medicines containing caffeine during therapy may result in exaggerated or prolonged effects of caffeine; if excessive cardiac or CNS stimulation occurs, caffeine intake should be reduced.
Other Drugs
Although taking ciprofloxacin extended-release tablets (a single 1-g dose) with omeprazole (40 mg once daily for 3 days) reduced peak plasma concentrations and area under the curve (AUC) by about 20%, the interaction was not considered clinically important. Concomitant use of ciprofloxacin and phenytoin has resulted in altered serum concentrations of phenytoin; caution is advised. Severe hypoglycemia has occurred rarely in patients receiving ciprofloxacin and glyburide.
Metoclopramide reportedly increases the rate of GI absorption of ciprofloxacin, while antimuscarinics (for example, scopolamine, pirenzepine) may delay GI absorption. Ciprofloxacin should be used cautiously in patients receiving drugs that depend on oxidative metabolism in the liver for elimination, particularly those with a narrow therapeutic range, since experience with xanthine derivatives indicates such interactions may be possible.
Acute renal failure occurred within 4 days after starting ciprofloxacin in a patient receiving maintenance cyclosporine therapy. The mechanism has not been clarified but could involve synergistic nephrotoxic effects and/or interference with cyclosporine metabolism. It has been suggested that using ciprofloxacin together with a nonsteroidal anti-inflammatory drug (NSAID) could increase the risk of CNS stimulation (for example, seizures), but more study and clinical experience are needed.